Accurate Coronavirus Information
& Safety Practices
Bottom line: The best way to reduce health and economic impacts is to:
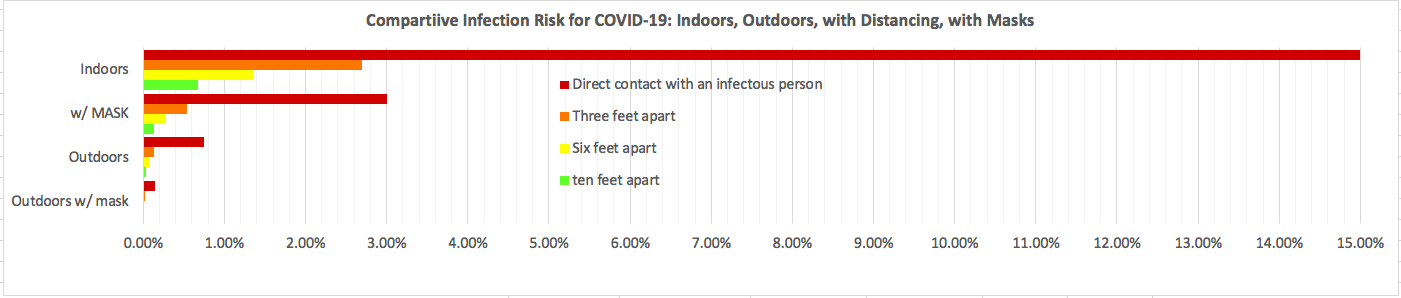
- Cover nose and mouth with a reusable cloth mask (85%± risk reduction)
- Physically distance (82% of the risk at 3 ft, 91% at 6ft 95% at 10ft)
- Connect outdoors (95%± risk reduction—if not outside, ventilate as much as possible; roll windows down)
- Eye protection, Wash hands, etc,
Wear a mask. Go outside to sociallze. Don't touch anyone but your partner, or people you are caretaking. Don't get within six feet of anyone else without covering your face with a reusable cloth mask. If you have disposable masks—donate them to your local hospital or clinic to keep health care workers at work).
These suggestions are based on a synthesis of all the latest science (see links above and below).
Breathing in droplets seems to be the main mode of transmission. The dose matters; you don't have to eliminate virus inhalation, just reduce it to where your immune system can fight it off.
Outside seems way better than originally theoretically thought, with few actual cases.
Aerosols appear more important than previously thought(tiny droplets that stay airborne in poorly ventialated indoor spaces for hours).
Surface transmission is seeming less important. The theoretical increased risk reduction value for combining masks and outdoors was obtained by multiplying the values for each studied individually; these havenot been studied together. It seems likely all the other stuff (surface disinfection, etc...) does not appear to weigh anywhere near as heavily as the first three.
What has changed? Because this is a novel virus, we had no emperical data, just theory and extrapolation. Now there is data from contact tracing, and we have the start of visibilty into how the virus transmits in the real world.
This is dynamic and may change again as more data comes in.
Details and rationale below—
Curated information on the pandemic and what to do. |
Practice 'Information Hygiene'
Avoid contracting or spreading the pandemic of misinformation about Covid 19. The useful, accurate information below has been carefully curated, and sanitized of misinformation.
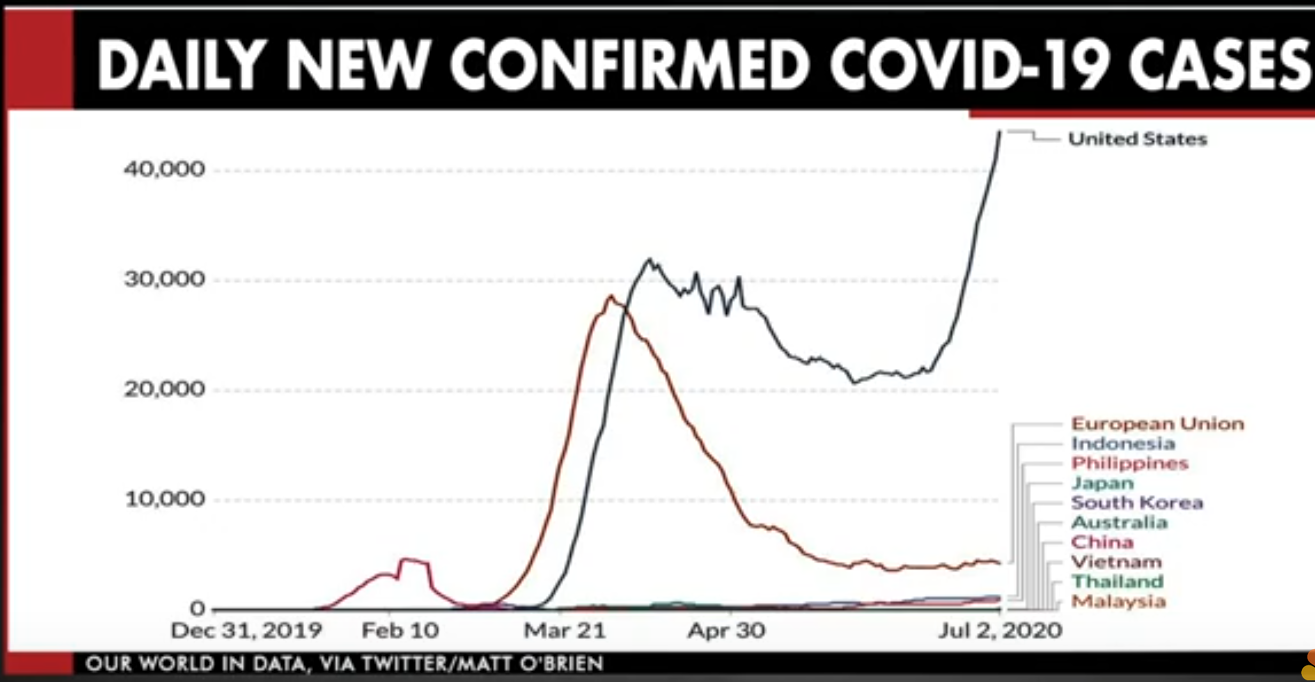
Look to most any other country to see how to better manage the pandemic than the US
For the first time in human history, an exponentially surging epidemic with community spread was reversed, in China (for now).
This was thought to be impossible. With a very aggressive approach, they got from 3,400 new infections per day January 2020, to just 24 new infections on March 11th, 2020.
Since then, Most of Europe, Slovakia, New Zealand, South Korea, and Singapore have contained the pandemic. Each used their own custom version of physical distancing, masks, handwashing, contact tracing, and quarentine of infected individuals.
What they all have in common: Science based, non-politicized reponse, public trust in leadership, and willingness of the clear majority of individuals to act in the common good.
What US, Brazil, and Russia have in common: politics-based, divisive response, non-science based, with low trust in government, universal confusion, and widespread pushback by large segments of the population.
More reading
- At the Canada-U.S. border, I encountered a study in contrasts—On one side of the border, almost everybody took the virus seriously—and few people had it. On the other, the reverse.
- Will the Pandemic Reshape Notions of Female Leadership?—Countries led by women have suffered six times fewer Covid-19 deaths than those led by men.
- The Best Global Responses to COVID-19 Pandemic
- New Zealand lifts all Covid restrictions, declaring the nation virus-free
- Lessons From Slovakia—Where Leaders Wear Masks

Slovakia's president, Zuzana ?aputová, and its nascent government administration, which came to power amid the pandemic, were among the first to model best practices for how to handle the outbreak—most notably by wearing protective masks and gloves for the government’s swearing-in ceremony.
The pandemic reveals US structural and cultural weaknesses we need to work on
Two days after Italy shut most of its economy down, in the US the headlines were "Trump defiant on testing and handshakes even as third Mar-a-Lago case emerges" and "Coronavirus is shutting down American life as states try to battle outbreak"
Years of wealth extraction from the health care system have left us with barely any more ventilators and hospital beds than were already in use before the pandemic in this active flu season. In Santa Barbara County, we may need several thousand intensive care beds, and we have several dozen, and this is a wealthy area.
Wealth extraction and concentration have left the social safety net thin and frayed.
The main risk of the coronavirus outbreak isn’t that you’re going to get sick and die, it’s that so many people are going to get sick so quickly that our healthcare services and infrastructure are going to be completely overwhelmed, with lots of collateral damage...and that our country
From the excellent article Coronavirus will radically alter the U.S, 3/19/2020:
What happens next in this pandemic depends largely on our government, health institutions and 327 million inhabitants — all making tiny decisions on a daily basis with outsized consequences for our collective future.
When Jason Christie, chief of pulmonary medicine at Penn Medicine, got projections on how many coronavirus patients might soon be flocking to his Philadelphia hospital, he said he felt physically ill. They saw how quickly the surge would overwhelm the system, forcing doctors to make impossible choices — which patients would get ventilators and beds, and which would die. “They were terrified. And that was the best-case scenario.”'
- America’s coronavirus response failed because we didn’t understand the complexity of the problem—it wasn't just Trump who got it wrong, there was a massive, pervasive shortage of systems thinking.
- We Are Living in a Failed State The coronavirus didn’t break America. It revealed what was already broken.
- Coronavirus is exposing all of the weaknesses in the US health system—High health care costs and low medical capacity made the US uniquely vulnerable to the coronavirus...America was less prepared for a pandemic than countries with universal health systems.
- How the White House Coronavirus Response Went Wrong
What to do to
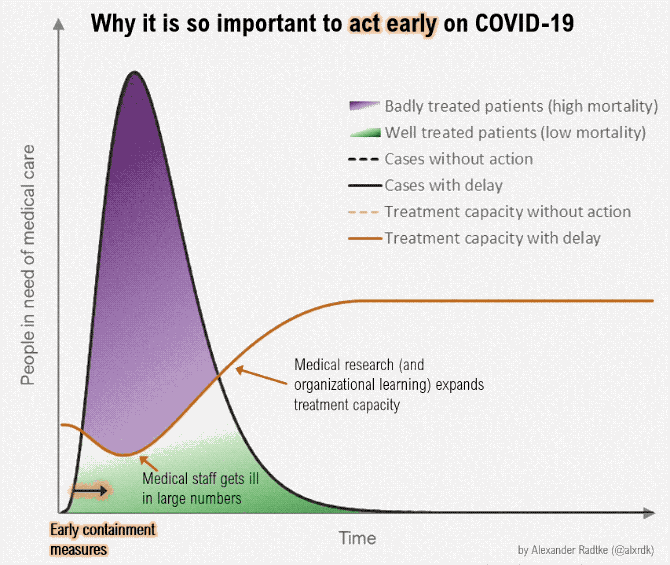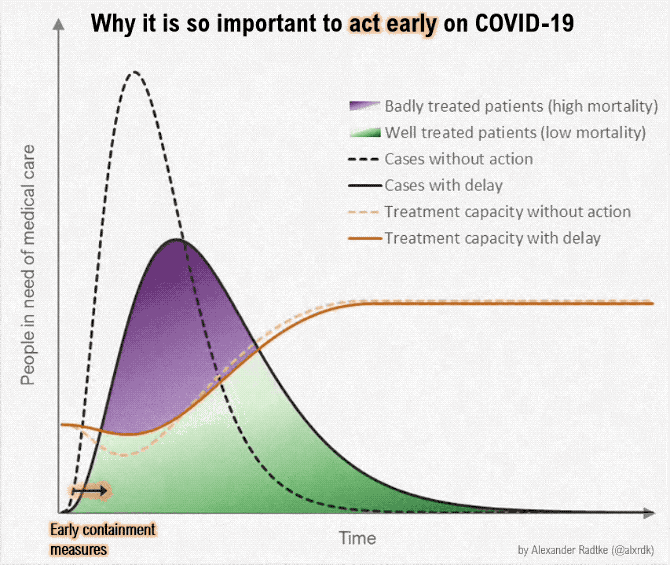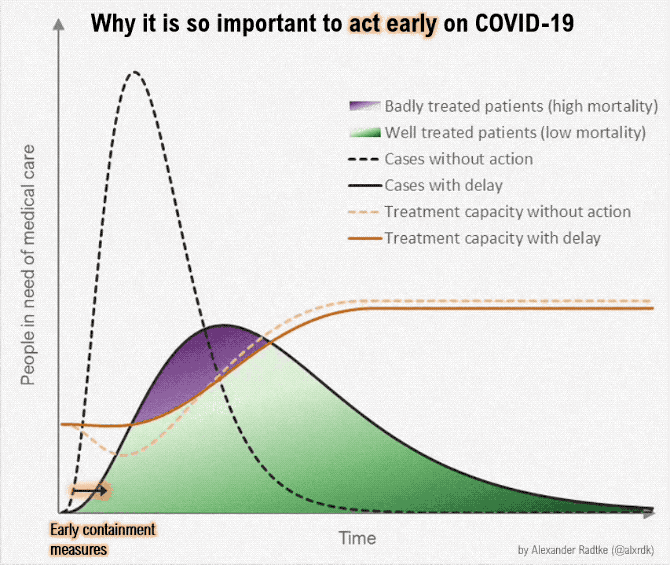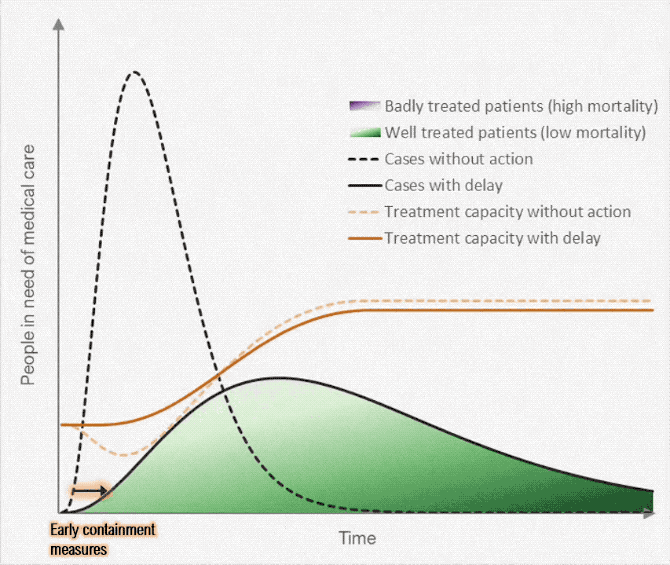
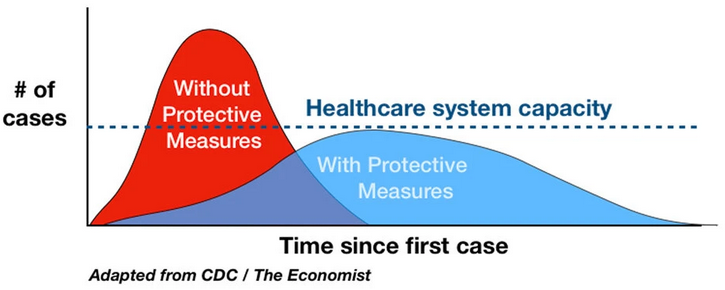
We have to flatten the curve for the rate of new infections vs time, so—
- health care resources don't get overloaded all at once. (The death rate is almost ten times greater when the health care system is overloaded; 0.5% vs 4-5%)
- testing and contact tracing can keep up
- schools and the economy can function more or less normally
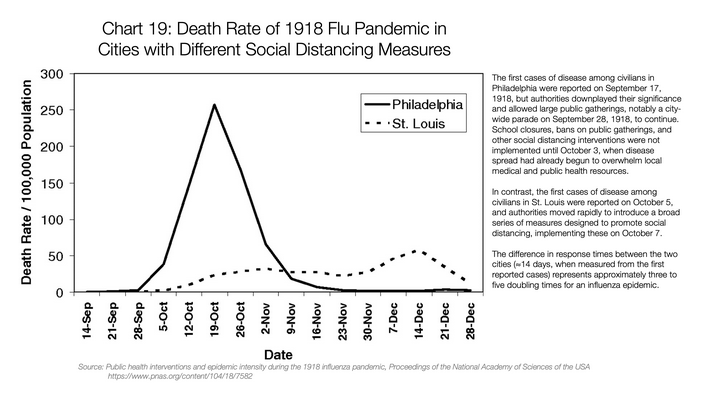
Philadelphia did not cancel a parade in the 1918 flu epidemic, St. Louis did:
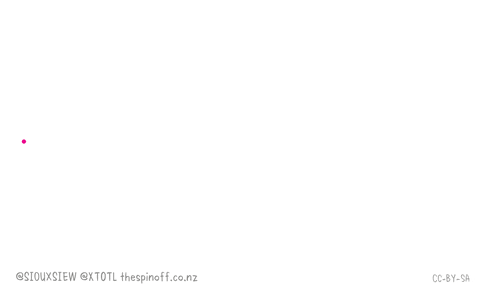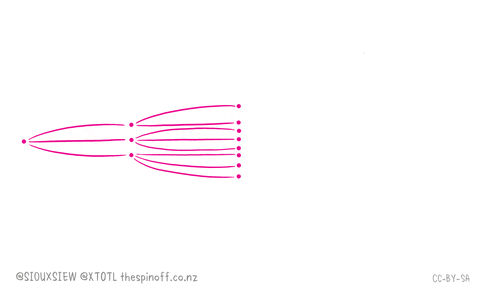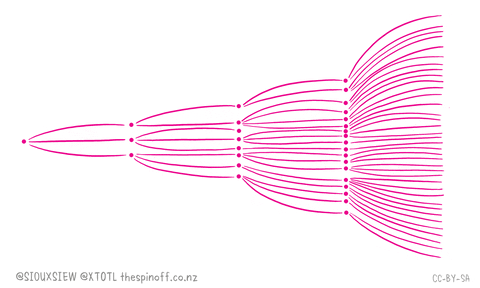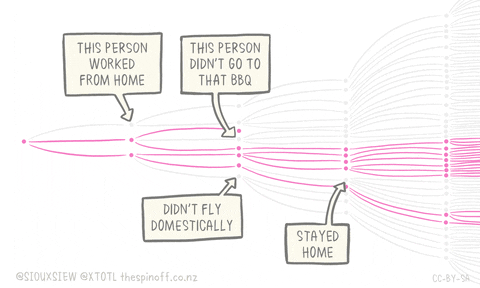
Bay Area is Flattening the Curve Early data indicates effectiveness of Shelter in Place
Suggested alert for your area:
ALERT: shelter in place and physical distancing required for pandemic safety. Stay >6’ from all but partner, your small children. If closer contact is required, cover face with cloth. Donate gloves, goggles, disposable masks to hospital or clinic. This is working to save lives elsewhere. Practice distance socializing for mental health and community cohesiveness.
Stay well ahead of the infection curve
These are in order of importance—
- Rigorously implement physical distancing—Now is the time to physically distance from people you love to protect them.I prefer physical distancing to "social distancing"...which sounds too close to "social isolation", which is its own health hazard. Family is kind of impossible to physically distance from past a certain point, which is why home isolation of sick people at home with family doesn't work well.
- Cover nose and mouth with a reusable cloth mask—to minimize transmission to/from yourself, help you to remember not to touch your face, and to send a message that helps others understand these are not normal times...without the social faux pax of wasting an N95 mask (see next item).
- If your work requires n95 masks, reduce and reuse them, and (after washing/ sterilization as needed) down-cycle them to the next, less critical use (washed N95 masks work pretty well for nasty construction dust, for example)
- Donate any N95 masks, gloves, eye protection to your local hospital or clinic where they can use it to keep from getting infected so they can keep working to save the life of you and people you love.
- Socialize outside
- Wash your hands— how to: video, poster in English, Cartella en Español, video en Español, Hands-Free-Handwash Hardware
- Think of others—if you are young and healthy, you're chance of needing and not getting a ventilator is smaller...but you might infect someone older or immunocompromised who winds up dying.
More reading—
-
Face masks critical in preventing spread of COVID-19—
-
NYT daily podcast Four new insights about the coronavirus
-
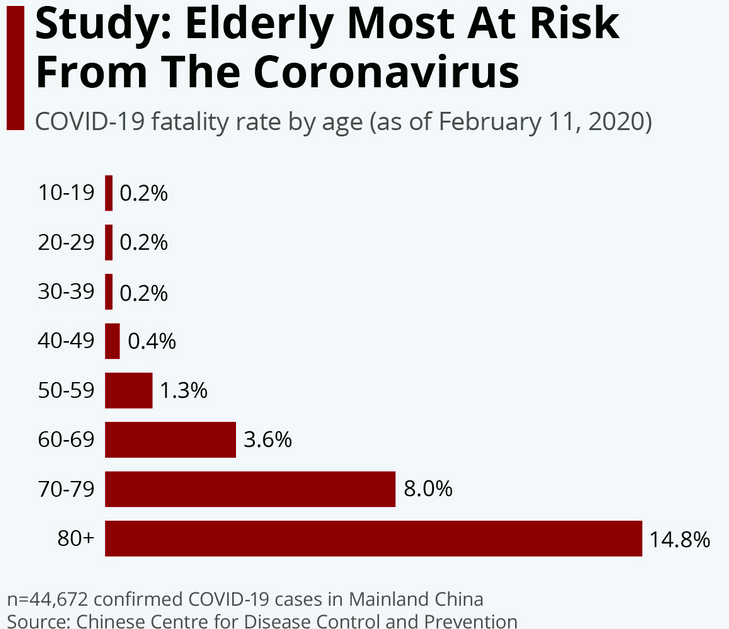
The coronavirus is killing far more men than women "we’re seeing another concerning trend, that the mortality in males seem to be twice in every age group of females"
Cover your nose and mouth...and help convert us to a face-covering culture
Places where mask wearing is culturally encouraged have slower infection spread
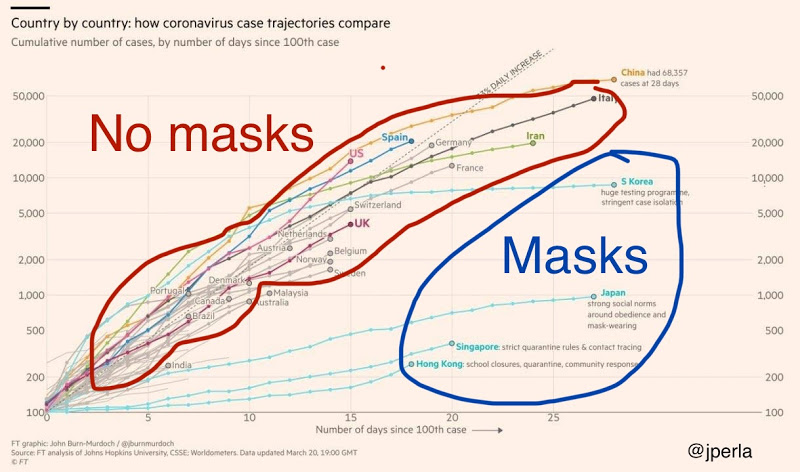
- Don't get near anyone else without wearing a bandana or homemade mask—especially if your work requires interacting face to face with the public, cover your nose and mouth so that you do not become an infection hub.
- If you have masks, don't wear them while there is a shortage, donate them to your local hospital or clinic—to keep health care workers at work.
- If 80 percent of people wear masks that are 60 percent effective, easily achievable with cloth...That’s enough to halt the spread of the disease—Research shows that even a cotton mask dramatically reduces the number of virus particles emitted from our mouths—by as much as 99 percent… Much of the confusion around masks stems from the conflation of two very different uses:...Masks can be worn to protect the wearer from getting infected or masks can be worn to protect others from being infected by the wearer. Protecting the wearer is difficult: It requires medical-grade respirator masks, a proper fit, and careful putting on and taking off. But masks can also be worn to prevent transmission to others, and this is their most important use for society. If we lower the likelihood of one person’s infecting another, the impact is exponential, so even a small reduction in those odds results in a huge decrease in deaths. Luckily, blocking transmission outward at the source is much easier. It can be accomplished with something as simple as a cloth mask. In Hong Kong, only four confirmed deaths due to COVID-19 have been recorded since the beginning of the pandemic, despite high density, mass transportation, and proximity to Wuhan. Hong Kong’s health authorities credit their citizens’ near-universal mask-wearing as a key factor (surveys show almost 100 percent voluntary compliance)… ...Taiwan ramped up mask production early on and distributed masks to the population, mandating their use in public transit and recommending their use in other public places—a recommendation that has been widely complied with. The country continues to function fully, and their schools have been open since the end of February, while their death total remains very low, at only six.
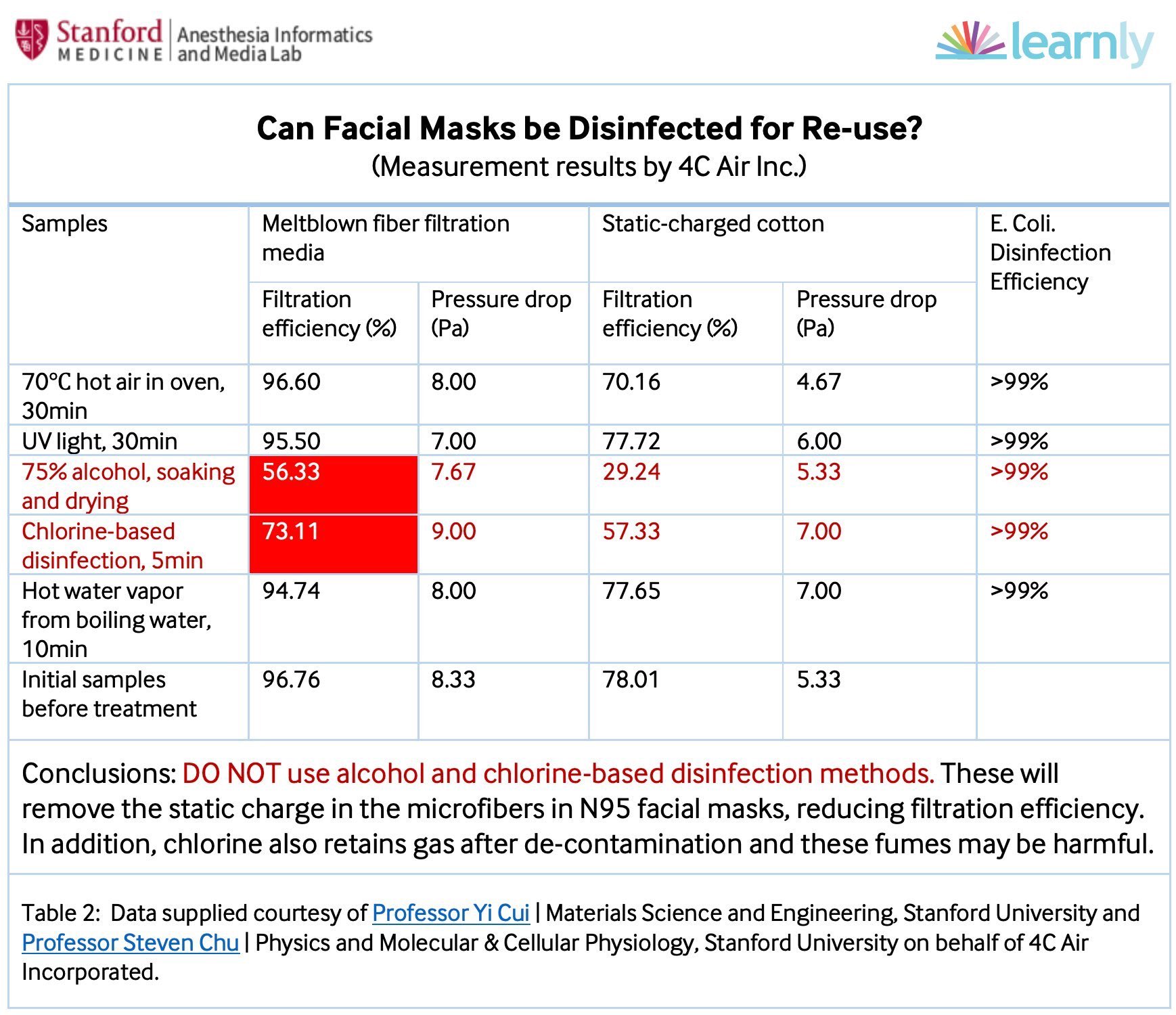
- Don't throw away any mask; reuse it sterilze and reuse it. Techniques that sterilize without overly compromising filtration:
- YES: 70 C / 158 F heating in a kitchen-type of oven for 30 min (up to 20 cycles)
- YES: Hot water vapor from boiling water for 10 min
- MAYBE: UV light 254 nm 30 min (10 cycles...may not reach deep into mask)
- MAYBE: hydrogen peroxide
- MAYBE: time leave the mask to sit in warm, dry conditions for 2+ days until the virus simply dies
- DON'T: microwave, use alcohol or chlorine, soak in soapy water, or heat over 70°C /160° F
- More info
- You need to wear a mask. Here’s how.
- Should I Start Wearing a Mask? The C.D.C. now recommends we cover our faces in public. Here is our guidance on how to best protect yourself, whether you have a mask or not.
- Everyone Thinks They’re Right About Masks
- New face mask guidance comes after battle between White House and CDC
- Universal mask-wearing is the most overlooked COVID-19 lifesaver
- Mask reuse (video)
Japan has the strongest mask-wearing culture in the world and one of the lowest COVID-19 infection rates

'Distance Socializing' and other ways to stay as healthy and balanced as possible
- Go outside—twenty times safer than inside
- Dance outdoors
- Encourage leaders to take this pandemic seriously, act boldly—to enforce physical distancing, and allocate public resources for health care and financial assistance. Socialized medicine is looking pretty good right now...
- Take heart; there is an upside to this—The Con Man presidency is probably over. Climate disrupting emissions are WAY down. More lives may well saved by these two factors than are lost in the pandemic. Animals are happier.
- The need for climate change action may be easier to communicate—now there's a way to talk about an invisibly growing exponential threat that suddenly explodes and massively disrupts the economy, society, and life itself...and for which early action is greatly rewarded.
- Cultivate deep, non-contact connection with your people, and check on them regularly—through face time or phone. Don't worry about screen time when it comes to video chatting with your family and friends. Get creative. Rather than hug, try standing a feet away, look each other in the eye, and tell each other what you appreciate about each other...
- Connect deeply with your spouse, kids—or others you can't physically distance from. Be curious about them and your connection, and connect more deeply and well.
- Connect with nature, get fresh air—It's only humans carrying this virus; this is the ideal time to commune with your other relations— the plants, animals, birds, flowing water and air, rocks and trees...
- Exercise—in nature if you can, dancing at home if you can't.
- Create screen-life balance when life has shifted to screens.
The best way to stay ahead of the curve is to reboot your brain in exponential pandemic mode
Our brains are wired for linear change; things drift, you make a change, then you don't have to pay attention for a while. That's not what's happening.
In an exponential situation, it seems like nothing is really happening for a long time, then maybe something, than wham! every day is a totally different deal than the day before. Gathering of under 250 people are OK, then 50, then 10 people a few days later, and then as close as you can get to zero. Then, the storm will pass, and we'll come out blinking in a different world.
If exponential change is what you expect, you will a) not be surprised, and b) be able to get ahead of the curve, help flatten it, stay within the capacity of the health care system, and reduce mortality by almost 10x.
| Parameter | Regular mode | Pandemic mode |
| Physical connection | Engage in healthy social touch | Act like a crazy (but effective) germaphobe; no hand shaking, no hugging, except with people in your innermost circle, until unless they or you become infected |
| Emotional connection | Regular level connection | Connect extra deeply and authentically |
| Handwashing | Save water, soap, and paper towels | Remove all virus possible |
| Travel, events | Live it up | Withdraw physically, reach out digitally |
| Mental model of change | Linear | Exponential |
What does keeping ahead of the exponential curve look like?
After a long, quiet incubation period, suddenly every day what makes sense is dramatically different than the day before, or the day after. With actual cases doubling about every 3 days, timely action makes all the difference:
instead of 10 Million cases in the United States if we wait 30 days, if we act 18 days sooner, we will have only 160,000 cases
Norway acted now, because it’s less economic impact to take drastic measures early than to do them later, and it saves a lot of lives and suffering by doing so. And Norway has only one confirmed death as of this writing.
Physical distancing must be ahead of the actual cases curve, which means being a week or so ahead of the reported cases curve:
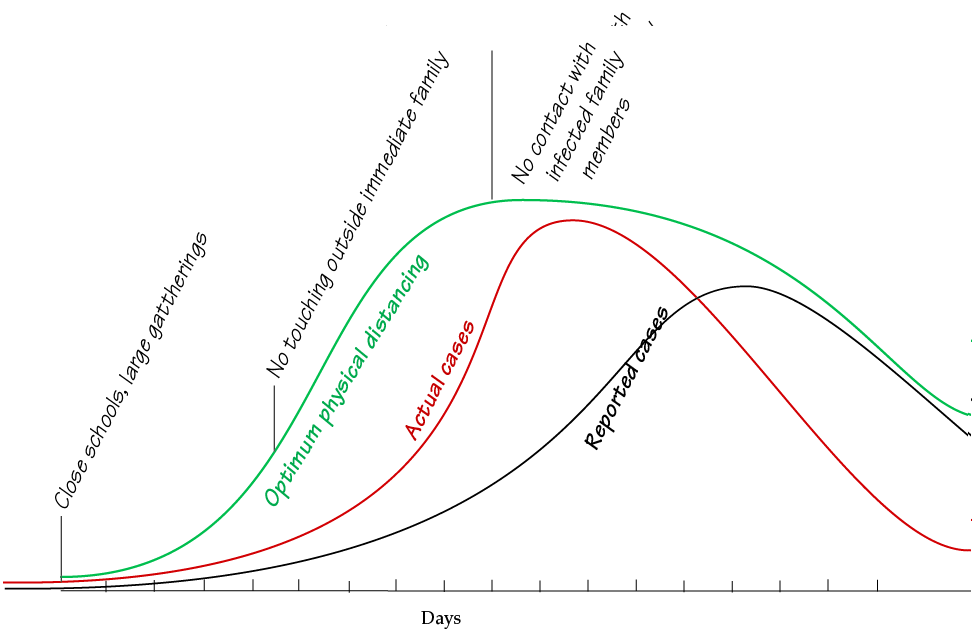
Here's what my days are like:
| Date | # reported cases in Santa Barbara County/ tests | Physical distancing effort | Pandemic mode |
| March 6 | 0 cases/ ? tests |
50% | Level 0-life as usual; with one more crisis that isn't discernibly affecting me. Last community dance with 50+ people, hugged, shook hands, and made PSA about handwashing technique and get ready. Barely washing hands after using bathroom. |
| March 11 | 0 cases/ ? tests |
75% | Level 1–dress rehearsal; practicing really washing hands, physical distancing, elbow bumps. Wondering if we should get more food, washing hands 15 x a day. |
| March 12 | 0 cases/ 7 tests |
80% | Level 2–preparation; buying last of food, soap, disinfectant, medicine; discussing plans with housemates, checking on family and friends, sounding the alarm in earnest. Washing hands 20 x a day, sometimes right after I just washed them, when I may have touched something some one else touched. Meeting 3 feet away from at risk (but still healthy) people we're checking on. No touching even with elbow. Lots of explaining. Touch of panic, able to push it back. |
| March 15 | 1 case/ 15 tests |
90% | Level 3–cocooning; hunkering down with immediate family and housemates. After going to the market for possibly the last time in 3 weeks, took off "around people" clothes and wallet and put them in a designated drawer, washed hands, showered, and wiped down phone with alcohol. Took two long walks in the fresh air with my partner; video chat with far away family. Trying to wrap my mind around these changes, and imagine what life will be like in a week. |
| March 16 | 2 cases/ 25 tests |
95% | Level 4–physical isolation; Setting up so we can split the house in two in case some of the four of us get sick. Not going around others physically at all. Exercising in the fresh air far from people, communicating for hours with friends and family remotely. |
| —I am guessing from here on out— | |||
| March 26 | 1,000 cases | 98% | Level 5–physical isolation between people with and without virus in same house; Separate bedrooms, bathroom, and provisional cooking facilities; mask on when interacting, constant online re-assurance of others, gratitude that water and power are still working. |
| June 21 | 200,000 cases | 75% | Level 1–post-pandemic; people coming out of physical isolation to meet in person again at last, and cope with worldwide economic recession, hopefully more galvanized to at last effectively deal with climate disruption, a far greater threat than the coronavirus pandemic. |
Transmission
- Transmission Methods (video; Anthony Fauci on Trevor Noah):
- Respiratory droplets, (coughing, sneezing) [2]
- Aerosols
- Mouth to hand to mouth (e.g., handshake)
- Fomites (infected clothes, furniture, sheets, hair, skin, vehicles, tools) [2]
- Fecal-Oral (ingesting infected fecal matter, flies landing on your food, touching your mouth with your hand after contact with a public door handle) [3]
- Possible airborne (different from droplets, airborne can be carried by dust in the air) [4]
- Understanding the virus and how to degrade it The following is from Irene Ken physician, whose daughter is an Asst. Prof in infectious diseases at Johns Hopkins University, quite informative:
- The virus is not a living organism, but a protein molecule (DNA) covered by a protective layer of lipid (fat), which, when absorbed by the cells of the ocular, nasal or buccal mucosa, changes their genetic code. (mutation) and convert them into aggressor and multiplier cells.
- Since the virus is not a living organism but a protein molecule, it is not killed, but decays on its own. The disintegration time depends on the temperature, humidity and type of material where it lies.
- The virus is very fragile; the only thing that protects it is a thin outer layer of fat. That is why any soap or detergent is the best remedy, because the foam CUTS the FAT (that is why you have to rub so much: for 20 seconds or more, to make a lot of foam). By dissolving the fat layer, the protein molecule disperses and breaks down on its own.
- HEAT melts fat; this is why it is so good to use water above 77 degrees Fahrenheit for washing hands, clothes and everything. In addition, hot water makes more foam and that makes it even more useful.
- Alcohol or any mixture with alcohol over 65% DISSOLVES ANY FAT, especially the external lipid layer of the virus.
- Any mix with 1 part bleach and 5 parts water directly dissolves the protein, breaks it down from the inside.
- Oxygenated water helps long after soap, alcohol and chlorine, because peroxide dissolves the virus protein, but you have to use it pure and it hurts your skin.
- NO BACTERICIDE OR ANTIBIOTIC SERVES. The virus is not a living organism like bacteria; antibodies cannot kill what is not alive.
- NEVER shake used or unused clothing, sheets or cloth. While it is glued to a porous surface, it is very inert and disintegrates only -between 3 hours (fabric and porous), -4 hours (copper and wood) -24 hours (cardboard), - 42 hours (metal) and -72 hours (plastic). But if you shake it or use a feather duster, the virus molecules float in the air for up to 3 hours, and can lodge in your nose.
- The virus molecules remain very stable in external cold, or artificial as air conditioners in houses and cars. They also need moisture to stay stable, and especially darkness. Therefore, dehumidified, dry, warm and bright environments will degrade it faster.
- UV LIGHT on any object that may contain it breaks down the virus protein. For example, to disinfect and reuse a mask is perfect. Be careful, it also breaks down collagen (which is protein) in the skin.
- The virus CANNOT go through healthy skin.
- Vinegar is NOT useful because it does not break down the protective layer of fat.
- NO SPIRITS, NOR VODKA, serve. The strongest vodka is 40% alcohol, and you need 65%.
- LISTERINE IF IT SERVES! It is 65% alcohol.
- The more confined the space, the more concentration of the virus there can be. The more open or naturally ventilated, the less.
- The Virus may persist on surfaces for up to 9 days, on some surfaces up to 27 days [5]...but this does not seem to equate to transmission.
- Incubation period: 2–14 days [1] 5-7 days, max 14
from forget about the death rate, this is why you should be worried about the coronavirus - Surfaces? Sneezes? Sex? How the Coronavirus Can and Cannot Spread (NYT)
- Can You Become Immune to the Coronavirus? It’s likely you can, at least for some period of time.
- More Americans Should Probably Wear Masks for Protection When researchers conducted systematic review of a variety of interventions used during the SARS outbreak in 2003, they found that washing hands more than 10 times daily was 55 percent effective in stopping virus transmission, while wearing a mask was actually more effective — at about 68 percent. Wearing gloves offered about the same amount of protection as frequent hand-washing, and combining all measures — hand-washing, masks, gloves and a protective gown — increased the intervention effectiveness to 91 percent.
- Simulating an epidemic This well-made video gives a sense of the math behind different pandemic interventions. Spoiler alert: while other interventions can flatten the curve and reduce overwhelm of the health system and mortality, identifying and isolating cases is the only way to reduce the total number of cases.
Stealth transmission is a thing
- Whole-town study reveals more than 40% of COVID-19 infections had no symptoms
- Up to 45 percent of SARS-CoV-2 infections may be asymptomatic
- 'Stealth transmission’ responsible for vast majority of cases, study says The explosive spread of the coronavirus in Wuhan, China, was driven by people whose disease was never diagnosed, a new study has found, suggesting that people with symptoms so mild that they may not have known they were sick unwittingly spread disease in China and ultimately around the world.
How do you tell if you have coronavirus?
Loss of smell and taste may be an early, distinguishing symptom of the novel coronavirus.
Here are the most common symptoms and the percentage of people who had them:
- Fever: 88%
- Dry cough: 68%
- Smell and/or taste loss 68% and 71%, respectively
- Fatigue: 38%
- Coughing up sputum, or thick phlegm, from the lungs: 33%
- Shortness of breath: 19%
- Bone or joint pain: 15%
- Sore throat: 14%
- Headache: 14%
- Chills: 11%
- Nausea or vomiting: 5%
- Stuffy nose: 5%
- Diarrhea: 4%
- Coughing up blood: 1%
- Swollen eyes: 1%
Help researchers: COVID Symptom Study on the App Store / Google Play
COVID-19 is a lower respiratory tract infection, which means that most of the symptoms are felt in the chest and lungs. That’s different from colds that bring on an upper respiratory tract infection, where you get a runny nose and sinus congestion. Those symptoms seem to be mostly absent for people with COVID-19, though they’re not unheard of.
The good news is that in China, most people who have gotten sick -- about 80% -- have had mild* to moderate symptoms.
Testing
Antibody Test, Seen as Key to Reopening Country, Does Not Yet Deliver The tests, many made in China without F.D.A. approval, are often inaccurate. Some doctors are misusing them. The rollout is nowhere close to the demand.
The virus test is often slow.
What to do if you get sick
If you start to show symptoms, call your doctor's office. Don’t go there before calling -- that might spread the infection around the doctor’s office. They may want to talk to you on the phone in a telemedicine visit.
Well...depends on where you are and what resources are available. With luck, there will be community resources marshalled to help you. Most likely if you are in the US, you will be mostly on your own—
- Self-quarantine will be far safer and more comfortable for everyone if people work out a plan before anyone in their household falls ill.
- Home isolation—keep your distance as much as possible, wear a bandana (your n95 masks should be donated to your hospital by now unless you are being cared for by an elderly person or some other high risk factor)
- 10 Things You Can Do to Manage COVID-19 at Home (Center for Disease Control video) OK, not great.
- Make sure someone knows you are sick and can help if you crash
- Fill out your advance care directive—What You Should Know Before You Need a Ventilator
What does the future hold?
There is a wave train of exponential curves coming our way
Including these:

- Actual Covid-19 infections (not shown)
- Reported Covid-19 infections (not shown)
- Health care system overwhelm, local collapse
- Covid-19 deaths
- Public awareness/ action
- Mental health crisis (not shown)
- Climate crisis — the big wave that we've been ignoring for decades
- Climate deaths—will likely be much lower thanks to the Covid-19 virus shocking people awake to the consequences of ignoring an exponentially growing, invisible threat until it is undeniable.
These curves are roughly, qualitatively right to give an idea of what's coming.
The only thing that matters now is the speed of your response
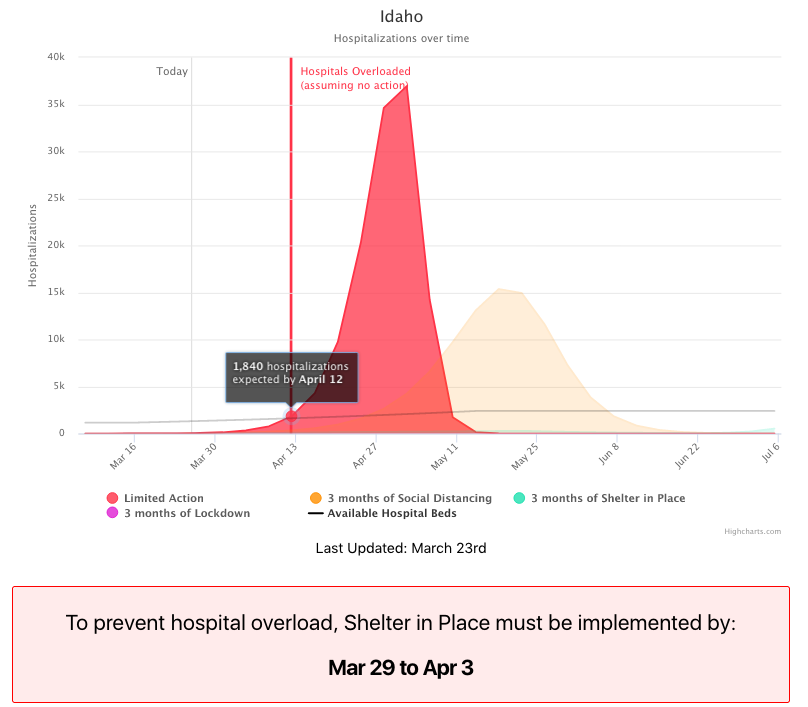
Animated covid-19 outbreak simulation with custom parameters
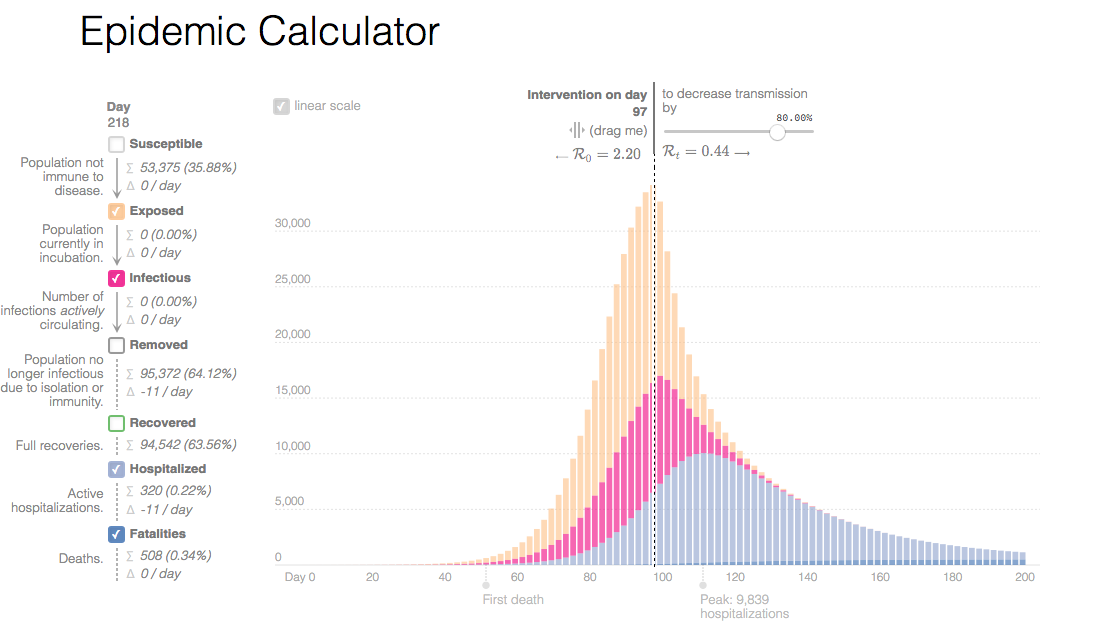
Epidemic Calculator with custom parameters
Timing is everything...start 50% sooner, get 98% fewer deaths!
...also, you can see that if you take timely action...it never looks like that action was warrented:
Start masking and distancing on day 100 ... 500± deaths in SB South Coast
Start masking and distancing on day 75...200± deaths in SB South Coast
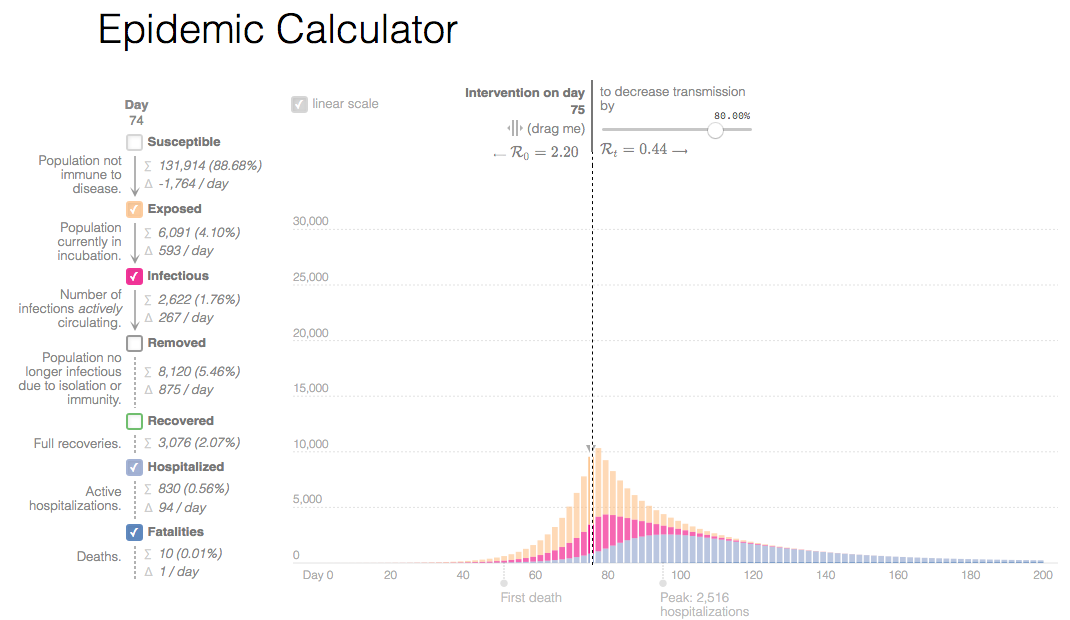
Start masking and distancing on day 50...8± deaths in SB South Coast
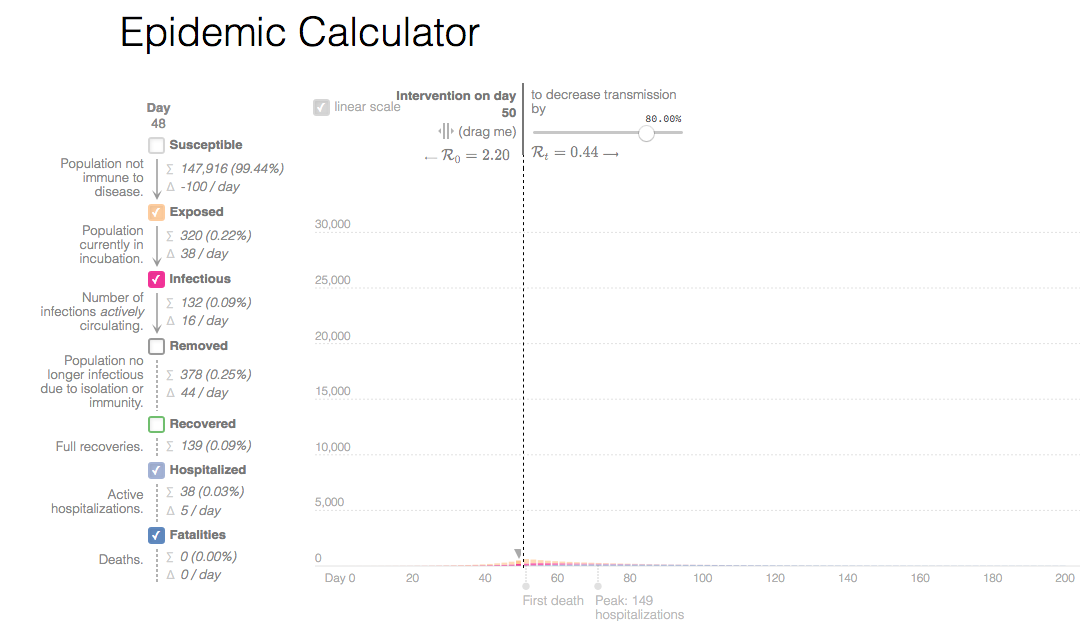
Estimated current infections should be the top line statistic and basis for decision making
Estimated current infections is roughly right as a basis for decision making Confirmed infections are 'preciscely wrong' as a basis for decision making The confirmed infections are a few weeks—about four doubling times—behind current actual infections. If testing is low, the numbers are even further off. Deaths are more accurate, but further out of date; around six doubling times.
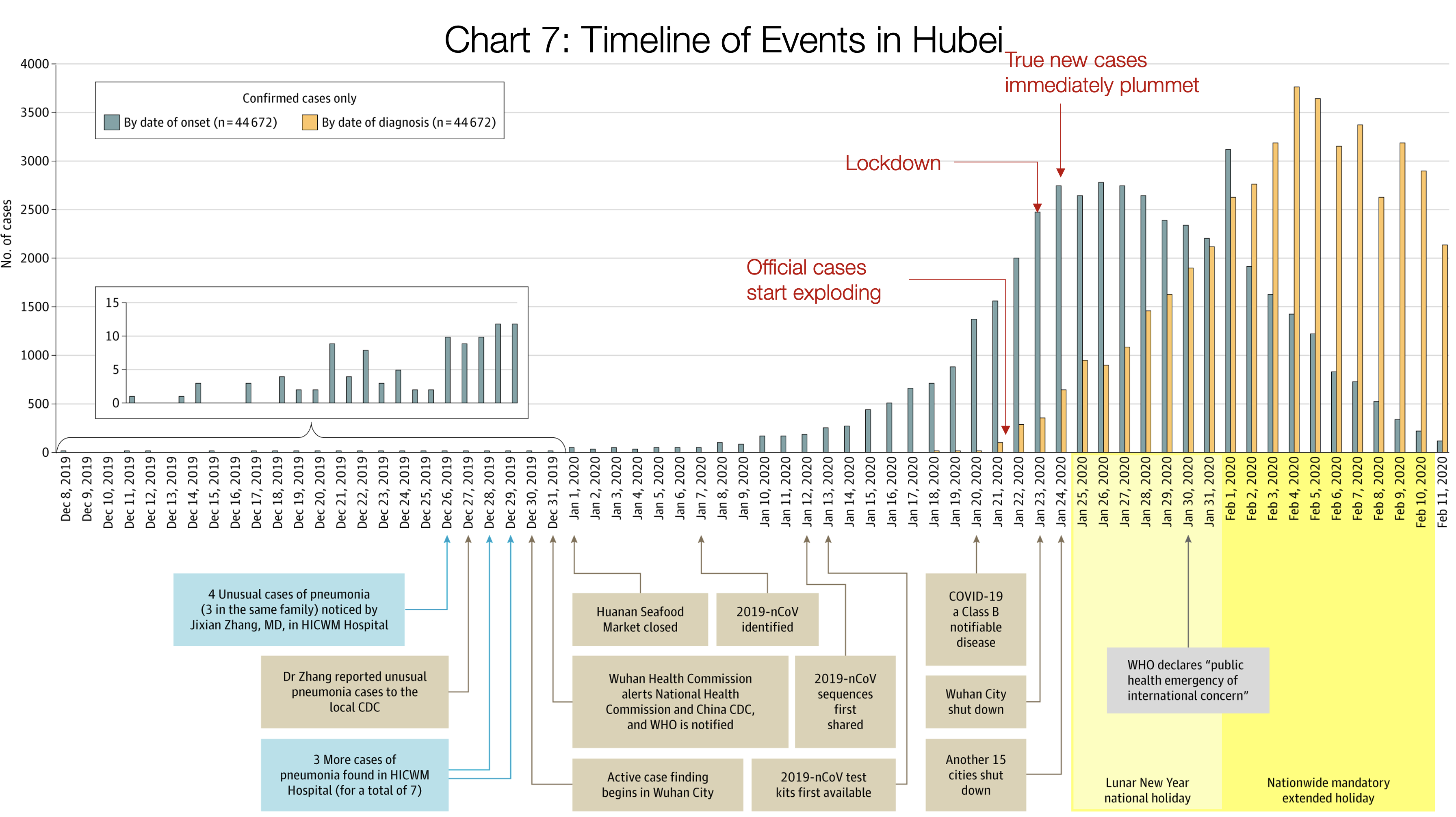
Timeline of events in Hubai graph and analysis. Note that true cases preceded official cases by 11±days
- Spreadsheet from Tomas Pueyo customized to calculate actual CA cases from CA deaths. You can copy this and make your own version.
- The Four Possible Timelines for Life Returning to Normal The coronavirus outbreak may last for a year or two, but some elements of pre-pandemic life will likely be won back in the meantime.
- The coronavirus isn’t a reason to put climate policy on hold. It’s a warning of the calamities ahead.
- We Can Safely Restart the Economy in June. Here’s How. Get tough now. Test widely to isolate those infected, and slowly revive businesses with workers and customers who have developed immunity.
- The pandemic could be a call to action on climate change "A good way to think about the coronavirus pandemic is that it is like climate change at warp speed."
More information
General
- The only thing that matters now is the speed of your response—graphs showing the current action status by state and probable outcome
- How to avoid COVID infection (Center for Disease Control video) OK, not great.
- US Center for Disease Control (CDC)
- California Department of Public Health
- The Dos and Don’ts of ‘Social Distancing’
- COVID-19 info (COVID-19 Pandemic Explained A Family Physician’s perspective on a new disease Leslie Waters MD, FAAFP)
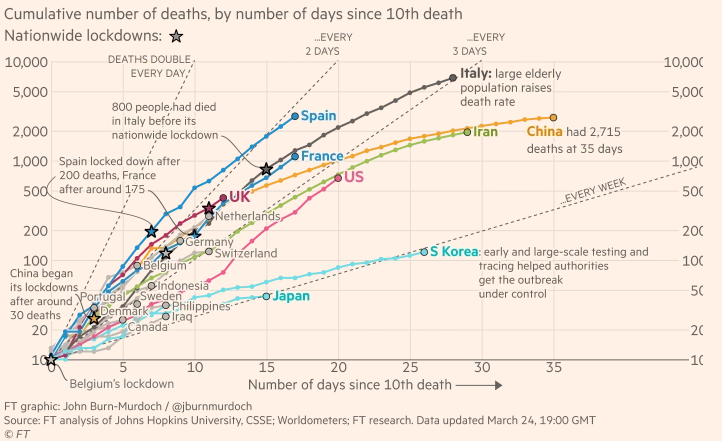
- Informative graphs from Financial Times of London
- Amazing interactive graphs
- World, National and State Statistics .don't pay too much attention to these numbers without reading the article below
- The Sober Math Everyone Must Understand about the Pandemic..the count of actual virus infections doubles every ~3 days. So we hear that the US only has 1573 cases today (3/12/20) [update as of 3/15/20: 3115 confirmed cases) and it doesn’t seem like a lot. It would be better to report the estimated actual cases, since reported cases don’t tell us much. However, we know from China that the actual number of cases are at least 10x greater than the reported cases, because people get infected and do not display symptoms.
Santa Barbara local info
- Safest place to buy groceries: Isla Vista Food Coop; exceptional attention to sanitation, and very few people in the store with UCSB closed, and excellent food at good prices. Please cover your face when shopping there or anywhere.
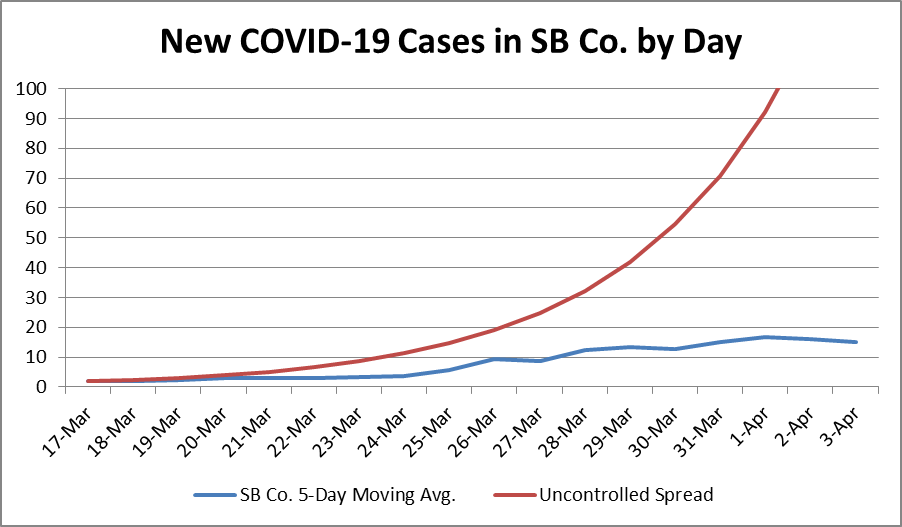
- Santa Barbara has substantially flattened its COVID-19 Curve Santa Barbara County began flattening its curve before the statewide stay at home order was issued and there are very early indications that it is now flat or even bent...My modeling shows that California will have substantial unused healthcare system capacity under the stay at home order.
- Cottage Infectious Disease Specialist Breaks Down the COVID-19 Virus and Pandemic A Must Watch for Understanding the Disease (Santa Barbara Independent)
- The SB Independent has a Coronavirus News page that also has the county statistics for the number of tests performed and number of people being monitored.
- Cottage Hospital has provided this informational and comprehensive clinical update presentation on Covid 19.
- Santa Barbara County Public Health Information Portal updated daily.
Reliable news
- NYT daily podcast (consider subscribing to support their good work)
- The Atlantic (consider subscribing to support their good work)
- Washington post
Mental and emotional health
- Interview with an anxiety specialist on how to relate with the current times mindfully.
- How to Work With Fear and Pain in a Moment of Crisis by Emily Horn
- The Great Unpatterning Continues. Make Sure You Take Advantage Of It. by Caitlin Johnstone
- Taking Care of Your Mental Health in the Face of Uncertainty by Doreen Marshall, Ph.D.
- 7 science-based strategies to cope with coronavirus anxiety by Jelena Kecmanovic
- The Neuroscience of Fear and 5 Helpful Tips by Rachel Posner
- Finding steady ground: strengthening our spirits to resist and thrive in these times
- Facing COVID-19 With Community Instead of Fear by Lornet Turnbull
- What Can the Coronavirus Teach Us? by Bill McKibben
- The Psychology Of Uncertainty: How To Cope With COVID-19 Anxiety by Bryan Robinson
- I survived solitary confinement. You can survive self-isolating
For government
- The only thing that matters now is the speed of your response—graphs showing the current action status by state and probable outcome
- What every mayor needs to know about the coronavirus from Seattle's mayor
 San Francisco a national model in fighting the pandemic
San Francisco a national model in fighting the pandemic- New Zealand’s Prime Minister May Be the Most Effective Leader on the Planet Jacinda Ardern’s leadership style, focused on empathy, isn’t just resonating with her people; it’s putting the country on track for success against the coronavirus.
- Convert manual drinking fountains, faucets to automatic/ hands free
- South Korea’s world-class response to COVID-19 is not the product of religion, or cultural destiny, but rather the result of diseases bested and crises weathered.
- Sewage Surveillance How many people have been infected with the new coronavirus? A group of Bay Area researchers aims to find out—by tracking what's in the local wastewater.
- Megan McArdle: When it comes to the coronavirus, we elites got it wrong. So did you populists.
- Landing at Dulles Airport, I encountered a case study in how to spread a pandemic I spent three hours in a jammed immigration hall trying to decide which analogy fit better: the ignorant Middle Ages during the plague years or the most chaotic airport in the least developed country...When he announced the travel ban, President Trump described it as an effort to keep out foreigners who might bring the virus to our shores. Instead, his actions caused an abrupt and dramatic influx of potentially infected people, with no attempt made to manage or control it. Dulles is a terrible, and terrifying, microcosm of a disaster magnified by incompetence.
For health care practitioners
- Keeping the Coronavirus from Infecting Health-Care Workers What Singapore’s and Hong Kong’s success is teaching us about the pandemic. [Summary] Here are their key tactics, drawn from official documents and discussions I’ve had with health-care leaders in each place. All health-care workers are expected to wear regular surgical masks for all patient interactions, to use gloves and proper hand hygiene, and to disinfect all surfaces in between patient consults. Patients with suspicious symptoms (a low-grade fever coupled with a cough, respiratory complaints, fatigue, or muscle aches) or exposures (travel to places with viral spread or contact with someone who tested positive) are separated from the rest of the patient population, and treated—wherever possible—in separate respiratory wards and clinics, in separate locations, with separate teams. Social distancing is practiced within clinics and hospitals: waiting-room chairs are placed six feet apart; direct interactions among staff members are conducted at a distance; doctors and patients stay six feet apart except during examinations. What’s equally interesting is what they don’t do. The use of N95 masks, face-protectors, goggles, and gowns are reserved for procedures where respiratory secretions can be aerosolized (for example, intubating a patient for anesthesia) and for known or suspected cases of COVID-19. Their quarantine policies are more nuanced, too. What happens when someone unexpectedly tests positive—say, a hospital co-worker or a patient in a primary-care office or an emergency room? In Hong Kong and Singapore, they don’t shut the place down or put everyone under home quarantine. They do their best to trace every contact and then quarantine only those who had close contact with the infected person. In Hong Kong, “close contact” means fifteen minutes at a distance of less than six feet and without the use of a surgical mask; in Singapore, thirty minutes. If the exposure is shorter than the prescribed limit but within six feet for more than two minutes, workers can stay on the job if they wear a surgical mask and have twice-daily temperature checks. People who have had brief, incidental contact are just asked to monitor themselves for symptoms.
- The nightmare of rationing health care Doctors and nurses need to talk now about the difficult choices ahead.
- ‘I've Been Walking Around for the Last Week Seeing What’s Coming’ A conversation with a physician on the front lines of the fight against the coronavirus ...Boston is one of the places that did take rapid and important action last week, such as delaying the Boston Marathon, closing Boston public schools, canceling our Saint Patrick’s Day parade. But as I walked around my neighborhood here yesterday, I was shocked and concerned to see that our coffee shops were full of people, our restaurants were full of people having drinks and enjoying their time together. And it just showed me that I am carrying a burden of seeing what we’re doing at the hospital, seeing how concerned we are about what we know is coming. But my fellow citizens don’t see it. My personal psychic crush is that I’ve been walking around for the last week seeing what’s coming and feeling somehow unable to share that clearly and effectively with friends, family..The only way we stop that situation from developing, the only clear way, is that our entire society sort of voluntarily commits—that’s the individual, the corporation, the public institution, town leadership, state leadership, and federal leadership—commit to slowing that process down so that we don’t have all of those patients beginning to crash the ICU beds at the same time..
For Manufacturers/ trades people
Needed:
- Split houses in two, with separate bedrooms, bathrooms, and provisional kitchens for healthy vs infected individuals
- Convert manual faucets, switches, doors to automatic/ motion sensor/ hands free versions
- Add handwash stations everywhere
- Ramp up production of components for hands free hardware
For businesses
Detailed analysis & more info
- 1918 Flu Pandemic historical documentary—We are having a luxury pandemic today by comparison-totally terrifying. San Francisco was a nationwide model then, too, BTW.
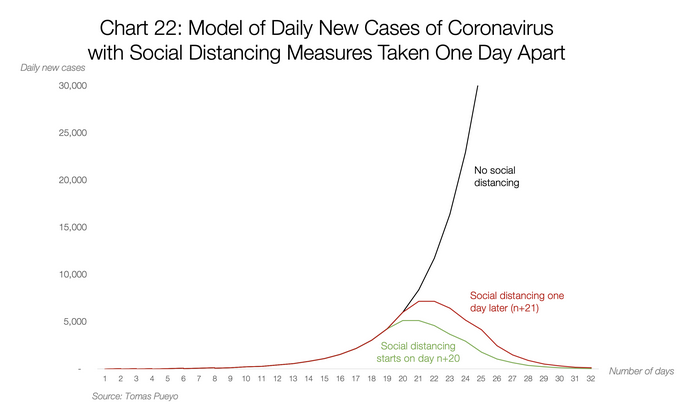
- These images summarize an excellent article by Tomas Pueyo, which was shared 28 million times in a week. The full article is a 24 min read.